Thoracic osteochondrosis is a chronic disease of the spine that causes degenerative-dystrophic changes in the intervertebral discs.
The thoracic spine is less often affected by osteochondrosis compared to the cervical and lumbar spine. This is because it is relatively inactive, stable and well strengthened by a muscle corset. Even rarer are the complications – bulging and herniated discs.
However, this disease is accompanied by extensive symptoms that significantly limit the quality of life and therefore require treatment. The use of medication only dulls the symptoms and provides a temporary effect that does not affect the development of the disease.
In order to reliably eliminate the symptoms, you need to influence the cause of the development of degenerative processes in the intervertebral discs. For this purpose, the clinic uses complex therapy, which produces positive results in more than 90% of cases. It includes methods of oriental reflexology and physiotherapy – acupressure, acupuncture, moxotherapy and other therapeutic procedures.
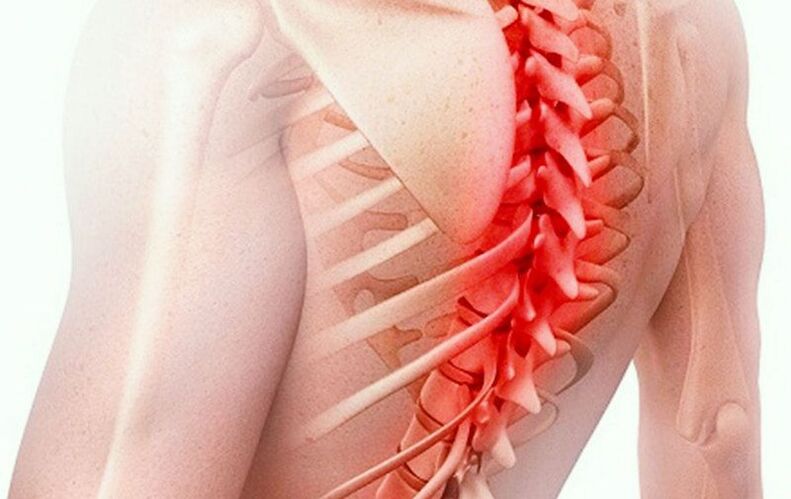
Symptoms, signs
Osteochondrosis occurs when the intervertebral discs flatten and the vertebrae grow together, leading to pinching of the spinal nerve roots. This results in pain between the shoulder blades (usually described as a pinching sensation).
The pain syndrome in thoracic osteochondrosis can be acute, intense or chronic, moderate.
In the first case, acute pain occurs suddenly and is called dorsago. In the second case, the pain is felt constantly, has an aching character and is called dorsalgia.
Irritation from a pinched root spreads along the nerve, radiates into the chest and becomes the cause of intercostal neuralgia - stabbing, cutting or burning pain in the chest that increases when inhaling, moving, coughing, sneezing, laughing.
Another characteristic symptom of thoracic osteochondrosis is pain in the heart area, which is accompanied by signs of cardioneurosis – heart palpitations, palpitations, increased heart rate.
A pinched nerve root leads to disruption of innervation, numbness, weakness of the hand, feeling of coldness in the hand, cyanosis (blue discoloration) or whitening of the skin. These symptoms are usually one-sided.
Pain in osteochondrosis can also radiate to the shoulder, under the shoulder blade and into the forearm.
Other symptoms of the disease include stiffness, tension in the back, numbness in the paravertebral area, shoulders, neck and collar area, difficulty breathing and a feeling of lumpiness in the chest.
The nerves that arise from the spinal cord in the thoracic region play an important role in innervating the entire body. Therefore, symptoms of osteochondrosis can appear in areas that seem unrelated to the spine. For this reason it is also called "chameleon disease".
These symptoms include:
- heartburn, flatulence,
- loss of appetite, nausea,
- digestive disorders (dyspepsia),
- Cough,
- cold feet,
- numbness in the body,
- pain in the right hypochondrium,
- discomfort in the abdomen,
- Sweat
In addition, thoracic osteochondrosis is manifested by impaired blood supply to the brain - headaches, pressure instability, dizziness, unsteady gait and loss of coordination.
Reasons for development, stages
The main role in the development of the disease is played by muscle spasms and tension (hypertonia) of the back muscles. These cramps occur with a sedentary lifestyle, poor posture, or prolonged stay in a static, uncomfortable position (e. g. , at a desk or while driving).
On the other hand, monotonous, heavy physical work also leads to persistent muscle cramps in the back (e. g. working with arms raised).
Muscle spasms impede blood flow and impede blood flow to the spine. This causes the nutrition of the intervertebral discs to deteriorate.
Intervertebral discs are shock-absorbing connective tissue cushions between the vertebrae. At the center of each disc is a mushy, semi-liquid nucleus that contains a lot of moisture. Water provides resistance to stress and resistance to pressure.
Each disc is reinforced with a rigid fiber ring along the outer circumference. The connective tissue of the intervertebral discs consists mainly of collagen - this substance is synthesized in the body and must be constantly supplied to the joints, intervertebral discs and other connective and cartilage tissues for their continuous regeneration.
Muscle spasms impair blood flow, resulting in not enough collagen reaching the discs for normal tissue repair. Lack of oxygen leads to a slowdown in metabolic processes.
Due to metabolic disorders, the tissue renewal of the intervertebral discs slows down and their wear accelerates. This leads to dystrophy and degenerative changes - the intervertebral discs become dehydrated, rupture, dry out, become flat and lose their shock-absorbing properties and elasticity.
Spasms in the back muscles are the main cause of overloading the spine in the thoracic region. If the intervertebral discs in the neck area are pressed by the increasing weight of the head due to poor posture and in the lumbar area by the increasing body weight due to excess weight, muscle cramps in the chest area play an exceptional role in the development of the disease. These spasms not only impede blood flow, but also tense the spine and compress the intervertebral discs both during the day and at night. The intervertebral discs are practically deprived of the opportunity not only for cell renewal, but also for simple rest and recovery. Therefore, when treating thoracic osteochondrosis, the first thing a doctor should do is relax the tense back muscles, eliminate muscle spasms and hypertension. Without this, effective treatment of the disease is impossible.
As the discs flatten, the gaps between the vertebrae become smaller, the vertebrae move closer together, and the nerve roots become pinched. This causes pain, which triggers a reflex muscle spasm and further increases the pressure on the intervertebral discs. Therefore, with the appearance of pain, the development of the disease usually accelerates.
These degenerative-dystrophic changes correspond to the first stage of osteochondrosis.
Important!
In old age, thoracic osteochondrosis usually develops against the background of general dehydration and metabolic disorders in the body. This is particularly evident in a decrease in height in older people, which occurs due to thinning of the intervertebral discs.
In the second stage, the outer fibrous ring becomes fiber-free. Its tissue becomes loose, weakened and it can no longer sustain the internal stress. This causes the intervertebral disc to bulge (usually locally) in the form of a protrusion.
A projection directed towards the spinal cord is called dorsal. Projections directed to the side are called lateral. The rarest case is a uniform protrusion of the intervertebral disc over the entire circumference.
The appearance of a bulge usually leads to increased pain. An X-ray clearly shows a decrease in the height of the gap between the vertebrae, as well as the development of osteophytes - bone outgrowths. They form on the edges of the vertebrae to compensate for the stress on the spine as the intervertebral discs become increasingly unable to cope with them.
In the third stage of the disease, the fibrous ring of the intervertebral disc can no longer withstand the internal pressure and tears. The resulting gap pushes out part of the nucleus pulposus of the intervertebral disc - resulting in an intervertebral hernia.
In the fourth stage of the disease, the range of motion in the back decreases sharply, the pain syndrome becomes constant and a comprehensive picture of neurological disorders develops.
diagnosis
At the first appointment, the doctor asks the patient about the symptoms and the circumstances of their occurrence, examines the medical history, conducts an external examination, paying attention to posture, the presence or absence of spinal deformities (scoliosis, kyphosis).
The cause of pain syndrome (dorsago, dorsalgia) can be both osteochondrosis and vertebral displacement (spondylolisthesis), ankylosing spondyloarthrosis, ankylosing spondyloarthrosis.
Osteochondrosis of the thoracic region is usually accompanied by muscle tension in the back and hypertonicity of the spinal muscles. The doctor performs palpation and applies sequential pressure to find pain points (trigger points) that correspond to the centers of muscle spasms.
To obtain more precise information, the doctor prescribes an X-ray or MRI scan.
X-rays for thoracic osteochondrosis provide the most general information - they help distinguish the disease from spondylolisthesis, detect osteophytes and narrow the gaps between the vertebrae.
Magnetic resonance imaging shows soft connective tissue better. With its help, the doctor can examine the structure of the intervertebral discs in detail, identify the protrusion, hernia (size, location, shape), as well as the condition of the ligaments, intervertebral joints, blood vessels, nerve roots, etc. see spinal cord stenosis (or its danger).
The doctor uses the MRI data to make a diagnosis and determine an individual treatment plan.
Treatment of osteochondrosis of the thoracic region
Drug treatments
To relieve back pain and intercostal neuralgia in thoracic osteochondrosis, nonsteroidal anti-inflammatory drugs can be used in the form of ointments, tablets or injections. The main effect of these drugs is anti-inflammatory, so their use is justified in cases where a pinched nerve root is accompanied by inflammation, that is, with thoracic radiculitis. NSAIDs also reduce inflammation of muscle tissue against the background of convulsions and persistent hypertension.
In acute pain syndrome, a paravertebral or epidural block can be used - an injection of an analgesic. In the first case, the injection is made in the place where the nerve root is pinched, in the second case in the area between the periosteum of the vertebra and the membrane of the spinal cord.
To relieve muscle tension and reduce pressure on nerve roots, blood vessels and intervertebral discs, muscle relaxants and antispasmodics are used.
Vitamin complexes are prescribed to nourish nervous tissue and prevent their atrophy.
To slow down the process of destruction of connective tissue, chondroprotectors can be prescribed.
These drugs have a symptomatic effect and can somewhat slow down the development of the disease, but in general they have almost no effect on the process of degenerative changes in the intervertebral discs.
Non-drug treatment
Non-drug treatment of thoracic osteochondrosis includes methods of physiotherapy, reflexology and physiotherapy.
The main goals of treatment are to relieve the inflammatory process, improve blood circulation and restore metabolic processes in the intervertebral discs, and stimulate cell renewal of connective tissue. For this purpose, the clinic uses complex therapy using methods of oriental medicine.
Important!
Physiotherapeutic exercises contribute to the formation and strengthening of the muscle corset, eliminate irrational loads on the spine and prevent congestion and muscle spasms.
surgery
In the case of large hernias, especially dorsal ones, with the risk of spinal cord stenosis and especially if these are present, surgical intervention - discectomy - may be indicated.
Part of the disc is removed or the entire disc is removed and replaced with a prosthesis. Although discectomy is a common surgical procedure, breast surgery is extremely rare.
Treatment in the clinic
Treatment of thoracic osteochondrosis in the clinic occurs in complex sessions that include several procedures – acupuncture, acupressure, moxotherapy, stone therapy, vacuum therapy, hirudotherapy for individual indications.
High efficiency is achieved through the synergy of individual methods and the elimination of the cause of the disease.
- Acupressure. By applying strong pressure to the trigger points of the back, the doctor eliminates muscle spasms, tension and congestion, improves blood circulation and restores unhindered blood flow to the spine. This reduces the load on the intervertebral discs and accelerates the processes of metabolism and tissue regeneration as the influx of oxygen and collagen increases.
- Acupuncture. Insertion of needles into bioactive points of the back, legs, arms, head and chest eliminates symptoms associated with impaired innervation – numbness, weakness in the arm. With the help of this procedure, intercostal neuralgia and other vertebral pain are relieved. In addition, acupuncture enhances the effects of acupressure and has anti-inflammatory and anti-edematous effects.
- Moxibustion therapy. Bioactive points in the spinal area are heated with a smoldering wormwood cigar. This procedure activates metabolic processes, increases blood flow to the intervertebral discs, stimulates and accelerates their recovery.
- Vacuum therapy. Cupping massage and cupping promote blood circulation and improve blood circulation.
- Manual therapy. By gently pulling the spine, the doctor relieves the pressure on the intervertebral discs, increases the distance between the vertebrae, releases compressed nerve roots, relieves pain and increases mobility in the back.
Gentle traction or traction is the only manual therapy technique indicated for thoracic osteochondrosis. Before starting, the doctor must thoroughly relax the back muscles, eliminate spasms and free the spine. The muscles are warmed up and relaxed with a massage. If this is not done, the application of physical exertion can result in injury - a fracture, sprain or fracture. Hardware methods of spinal traction in osteochondrosis are ineffective and even dangerous, therefore they are not used in clinic.
Hirudotherapy
The placement of medicinal leeches improves local blood circulation, blood flow to the intervertebral discs and has an anti-inflammatory effect.
Stone therapy
Smooth stones heated to a certain temperature are placed along the spine to deeply warm and relax the spinal muscles, improve blood circulation and stimulate blood circulation.
The duration of a treatment session in the clinic is 1–1. 5 hours, depending on the individual indication. The course of treatment usually includes 10-15 complex sessions. Once completed, a follow-up MRI will be performed to evaluate the treatment results achieved.
Complications
The main complication of thoracic osteochondrosis is stenosis of the spinal cord due to a herniated disc with the development of body paralysis.
Other possible complications are associated with disruption of the innervation of the body by pinching the spinal nerve roots: the development of diseases of the gastrointestinal tract, kidneys, heart and reproductive system.
prevention
To prevent the development of thoracic osteochondrosis, you should avoid a sedentary lifestyle and monitor your posture.
Important!
If a child or adolescent suffers from scoliosis, it is advisable to cure this disease without hoping that it will go away on its own. A lateral curvature of the spine occurs as a growing pain but can last a lifetime.
In this case, persistent muscle tension and spasms are inevitable, which in turn leads to the development of osteochondrosis and possibly its complications. In addition, scoliosis itself is fraught with complications from the respiratory, digestive and cardiovascular systems.

















































